Richfield (435) 896-6497
Ephraim (435) 283-4076
May 2024
Cuboid Syndrome
Cuboid syndrome mostly affects athletes, although it can affect non-athletes too. It is also known as cuboid subluxation or cuboid fault syndrome. This condition occurs when joints and ligaments near the cuboid bone of the foot are damaged, or when the cuboid bone itself is dislodged from its natural position. It is usually marked by pain on the outer side of the foot, which may be persistent or may come and go. Cuboid syndrome can be difficult to diagnose unless it becomes severe and more noticeable. Your doctor will likely ask questions about when the pain began and how long it has been present, and will put pressure on the cuboid bone to determine if that area is the origin of the pain.
Causes of Cuboid Syndrome
- Any repetitive stresses placed on the foot due to athletic activities are a common cause of cuboid syndrome.
- Although it develops over time, it is possible that this syndrome can occur all of sudden due to a single event or injury.
- Over-pronation can exacerbate the condition if not corrected.
Disagreements Amongst Podiatrists Regarding Cuboid Syndrome
- Some refer to it as the dislocation of the calcaneal-cuboid joint only.
- Other podiatrists see it as an injury of the ligaments located nearby, which also involves the cuboid bone.
It is very important that when you experience any kind of pain on the side of your foot, you should seek medical care right away. If a subluxed cuboid is caught early, your feet may respond well to the treatment, and you can get back into sports or other activities again as soon as the pain subsides.
Cuboid Syndrome in Athletes
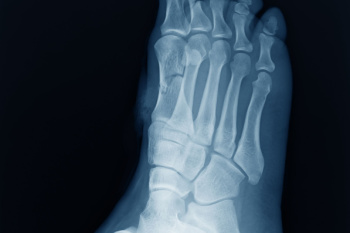 Cuboid syndrome is a condition where the cuboid bone, located on the outer side of the midfoot, becomes partially dislocated or misaligned. This often occurs due to injury or repetitive strain. Athletes are more likely to get cuboid syndrome than other groups because their activities, such as running or jumping, put significant stress on the foot's complex structures. This is especially true for those in sports requiring sudden changes of direction or explosive movements. Symptoms of cuboid syndrome may include intense lateral foot pain, redness, and swelling. A podiatrist, or foot doctor, can treat cuboid syndrome through manual manipulation to realign the bone, along with rest, compression, and elevation to reduce inflammation. Additionally, the use of taping techniques and custom orthotics may help stabilize the cuboid bone and prevent recurrence, allowing athletes to return to their activities with reduced risk of further injury. If you suspect cuboid syndrome, it is suggested you make an appointment with a podiatrist as soon as possible.
Cuboid syndrome is a condition where the cuboid bone, located on the outer side of the midfoot, becomes partially dislocated or misaligned. This often occurs due to injury or repetitive strain. Athletes are more likely to get cuboid syndrome than other groups because their activities, such as running or jumping, put significant stress on the foot's complex structures. This is especially true for those in sports requiring sudden changes of direction or explosive movements. Symptoms of cuboid syndrome may include intense lateral foot pain, redness, and swelling. A podiatrist, or foot doctor, can treat cuboid syndrome through manual manipulation to realign the bone, along with rest, compression, and elevation to reduce inflammation. Additionally, the use of taping techniques and custom orthotics may help stabilize the cuboid bone and prevent recurrence, allowing athletes to return to their activities with reduced risk of further injury. If you suspect cuboid syndrome, it is suggested you make an appointment with a podiatrist as soon as possible.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Dr. Blake Zobell from Utah. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact one of our offices located in Richfield and Ephraim, Utah . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Are Bunions?
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
How Bunions Develop
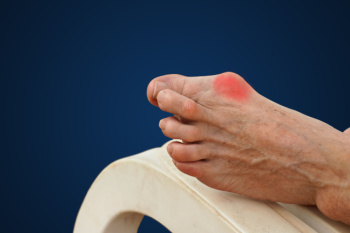 Bunions, medically known as hallux valgus, are bony bumps that form at the base of the big toe. They develop when the bones in the front part of the foot move out of place, while the tip of the big toe pulls toward the smaller toes. This forces the joint at the base of the big toe to stick out. Over time, the movement of the big toe toward the others creates a noticeable bump, which can become painful due to inflammation or arthritis within the joint. It may require treatment ranging from padded shoes and orthotics to surgery. Certain people are genetically predisposed to develop bunions, whereas other cases of bunions may develop due to ill-fitting footwear. High heels or shoes with a narrow toe box can exacerbate this condition. Additionally, conditions like arthritis can also contribute to bunion development by weakening and damaging the cartilage in the joint. If you have a bunion, it is suggested that you visit a podiatrist for treatment options and to prevent it from worsening.
Bunions, medically known as hallux valgus, are bony bumps that form at the base of the big toe. They develop when the bones in the front part of the foot move out of place, while the tip of the big toe pulls toward the smaller toes. This forces the joint at the base of the big toe to stick out. Over time, the movement of the big toe toward the others creates a noticeable bump, which can become painful due to inflammation or arthritis within the joint. It may require treatment ranging from padded shoes and orthotics to surgery. Certain people are genetically predisposed to develop bunions, whereas other cases of bunions may develop due to ill-fitting footwear. High heels or shoes with a narrow toe box can exacerbate this condition. Additionally, conditions like arthritis can also contribute to bunion development by weakening and damaging the cartilage in the joint. If you have a bunion, it is suggested that you visit a podiatrist for treatment options and to prevent it from worsening.
If you are suffering from bunions, contact Dr. Blake Zobell of Utah. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact one of our offices located in Richfield and Ephraim, Utah . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Managing Peripheral Artery Disease
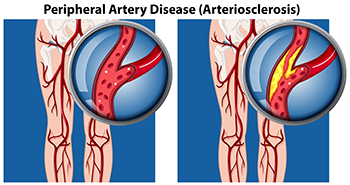
Peripheral artery disease, or PAD, particularly affects people with type 2 diabetes. Peripheral artery disease is often mistaken for normal aging or arthritis, but in fact it is the result of a build-up of fatty deposits in the arteries that restricts blood supply to the lower limbs and feet. Leg pain during exercise that persists with rest could signal PAD, necessitating evaluation by a podiatrist. Risk factors such as diabetes, smoking, and high cholesterol significantly contribute to PAD. Regular check-ups with a podiatrist, especially for diabetic individuals, are essential for assessing and managing foot health. One side effect of peripheral artery disease is the inability of wounds to heal properly, putting the patient at risk for foot ulcers. Early detection and intervention is essential, as such open wounds can deteriorate into gangrene and increase risk of limb loss if left untreated. For that reason, symptoms like persistent leg pain or slow-healing wounds require prompt medical attention from a podiatrist. If you are experiencing symptoms of peripheral artery disease, it is suggested that you add a podiatrist to your team of healthcare professionals.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Blake Zobell from Utah. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Richfield and Ephraim, Utah . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Why Live with Pain and Numbness in Your Feet?
Blisters
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
Treating Blisters on the Feet
 Blisters on the feet commonly develop due to friction and pressure. This can occur when wearing new or ill-fitting shoes, or from intense activities like running or hiking. Blisters are small pockets of fluid that form under the skin to cushion and protect deeper tissues from damage. While blisters often heal on their own, improper care can lead to infection and further complications. A podiatrist can help manage blisters on the feet, both by treating existing blisters and helping with prevention techniques. They can safely drain large or painful blisters in a sterile environment, apply appropriate dressings, and prescribe topical treatments to prevent infection. Additionally, podiatrists can provide valuable advice on selecting the right footwear and using special padding or insoles to reduce friction points. Podiatrists may also recommend specific socks or taping techniques to protect sensitive areas of the feet, which can prevent future blisters and ensure healthy foot care practices. If you have painful or recurrent blisters on the feet, it is suggested that you make an appointment with a podiatrist.
Blisters on the feet commonly develop due to friction and pressure. This can occur when wearing new or ill-fitting shoes, or from intense activities like running or hiking. Blisters are small pockets of fluid that form under the skin to cushion and protect deeper tissues from damage. While blisters often heal on their own, improper care can lead to infection and further complications. A podiatrist can help manage blisters on the feet, both by treating existing blisters and helping with prevention techniques. They can safely drain large or painful blisters in a sterile environment, apply appropriate dressings, and prescribe topical treatments to prevent infection. Additionally, podiatrists can provide valuable advice on selecting the right footwear and using special padding or insoles to reduce friction points. Podiatrists may also recommend specific socks or taping techniques to protect sensitive areas of the feet, which can prevent future blisters and ensure healthy foot care practices. If you have painful or recurrent blisters on the feet, it is suggested that you make an appointment with a podiatrist.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Dr. Blake Zobell of Utah. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
- Bubble of skin filled with fluid
- Redness
- Moderate to severe pain
- Itching
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact one of our offices located in Richfield and Ephraim, Utah . We offer the newest diagnostic and treatment technologies for all your foot care needs.









